|
Measles is a highly infectious disease caused by a virus. It is spread either via droplets or the air when an infected person breathes, sneezes or coughs. It can lead to serious complications such as pneumonia, encephalitis (inflammation of the brain) and death. Measles infection also damages and suppresses the whole immune system, so people who have had measles are more likely to catch other infectious diseases. This effect can last for as many as three years after they recover from measles. In high-income regions of the world, such as Western Europe, measles still causes death in about 1 in 5000 cases. But in the poorest regions, as many as 1 in 100 will die. Before widespread vaccination was introduced, the disease caused an estimated 2.6 million global deaths each year. And worldwide, measles is still a major cause of death. In 2016 about 90,000 people died of measles, although this was the first year on record when global measles deaths fell below 100,000 a year. However, following these years of decline, when vaccination dramatically reduced the number of deaths, in 2022 measles cases rose by 18%, and deaths by 43%, compared with 2021. During this time, worldwide vaccination coverage also declined to its lowest level since 2008. See this World Health Organization and Centers for Disease Control and Prevention report. Since a measles vaccine was introduced in the UK in 1968, the UK Health Security Agency estimates that 20 million measles cases, and 4,500 deaths, have been averted. Although measles transmission was briefly stopped in the UK altogether in 2016 and 2017, it re-started in 2018. It stopped again during the COVID-19 pandemic. However, during 2023 cases increased once again, and have since continued to grow, especially in the West Midlands and London areas of the country. Between 1 January 2023 and 30 June 2023, there were 128 cases of measles in England, compared with 54 cases in the whole of 2022. The year 2024 saw 2,911 confirmed cases in England, the highest since 2012. The outbreak has continued into 2025, with 420 cases confirmed between January 2025 and the end of May Most cases have been in unvaccinated children, under the age of 10. At the start of 2024, the UK Health Security Agency declared a national incident, and urged parents to get their children vaccinated against measles, if they weren’t already. Two doses of vaccine are highly effective in preventing infection.
The World Health Organization also issued an urgent warning over the very large increase in measles cases across Europe. |
Measles
Infectious Disease
|
Measles usually starts with cold-like symptoms, red eyes and sensitivity to light, a high temperature, and greyish-white spots in the mouth and throat. A red-brown rash usually appears a few days later, spreading from behind the ears to the rest of the body. A child with measles will have to spend about five days in bed and could miss two weeks of school. Even in wealthier countries such as the UK, around one in every 15 children with measles will develop more serious complications. These can include:
In countries like the UK, measles causes death in about 1 in 5000 cases. In rare cases, measles can lead to a condition called SSPE (subacute sclerosing panencephalitis). SSPE is a persistent viral infection, a devastating complication of measles which leads to a progressive destruction of the central nervous system. Symptoms can develop years after the initial infection. It results in dementia, loss of motor control, epilepsy and eventually death. A US study has suggested that SSPE may be more common than previously thought. Do watch the short film in the video section below: 'SSPE - a serious complication of measles: Sarah Walton's story'. |
|
Measles is spread through the air or water droplets, breathed, coughed or sneezed by infected individuals. People who have measles are infectious from when the first symptoms appear until four days after the rash appears. NHS advice for anyone who thinks they may have measles is to stay at home and call their GP for an urgent appointment or NHS 111. This reduces the risk of measles being spread to vulnerable people, such as young babies, people who are pregnant, and those with weakened immune systems. Measles is one of the most infectious diseases; if a child who is not immunised comes into contact with someone who has measles, it is very likely that they will catch the disease and risk developing serious complications, as the graphic below, from the US Centers for Disease Control and Prevention, shows.

Measles is highly contagious
|
|
The recommended way to protect your child is vaccination with the MMR vaccine. In the short film below, experts talk about measles and its complications, and the importance of the MMR vaccine.
Measles and the MMR vaccine
https://www.youtube.com/embed/gvJIQaXMCxY?wmode=opaque&controls=&rel=0
A life changed by measles: Sarah Clow's storySarah Clow fell seriously ill with measles when she was five and was left with lasting disabilities including deafness, partial sight and learning difficulties. Her mother Audrey talks about the impact this has had on Sarah and the whole family. Thanks to Rockhopper TV for the original footage. Sarah was not vaccinated against measles as a child because she had had eczema. Advice on this has now changed; current advice is that children with eczema can safely receive the MMR vaccine and other vaccines.
SSPE - a serious complication of measles: Sarah Walton's storySarah Walton caught measles when she was 11 months old, and at the time recovered well. Twenty four years later, however, she fell ill and was diagnosed with subacute sclerosing panencephalitis (SSPE). This is a rare but devastating complication of measles which leads to a progressive destruction of the central nervous system. In this video Sarah’s mother Jo talks about the impact that SSPE has had on Sarah and the people around her. For more information about the egg allergy issues raised in the video, click here.
|
How measles damages the immune systemAs well as causing serious disease, the measles virus attacks the white blood cells that protect us against other diseases. During any infection by bacteria or viruses, our immune system makes antibodies to fight the disease. For many diseases, an 'immune memory' is then created in special white blood cells called T lymphocytes. If we come into contact with that disease again, these cells will 'remember' it and react quickly to fight it, so that we do not become ill. However, measles infection destroys these special white blood cells, wiping out our immunity to diseases we have already had. This makes it much more likely that people who have had measles will catch other infections, even ones they have had before. Research published in 2015 Measles cases before and after vaccination in the UKThe graph below shows reported numbers of measles cases in the UK between 1940 and 1995. Before a vaccine existed, there were often hundreds of thousands of measles cases every year. In 1967, the year before a vaccine was first introduced, there were 460,407 suspected cases of measles in the UK, and 99 people died from the disease. By the end of the 1980s, vaccination had brought these figures down to around 10,000 suspected cases a year, with one or two deaths, and since then measles cases have fallen still further. 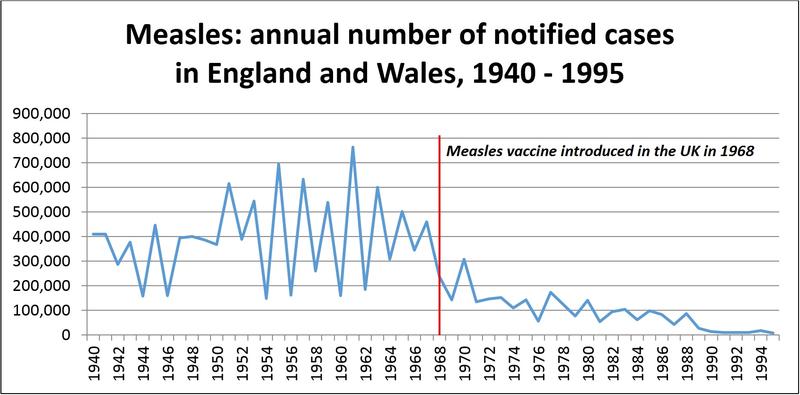
Click here for an accessible text version of this graph Data source: UK Health Security Agency However, the number of children receiving the MMR vaccine dipped in the 2000s, and as a result there have been several outbreaks of measles in the UK.
See the UK Health Security Agency page on measles deaths for full details of measles deaths since 1980. The graph below shows the numbers of measles cases in England between 1996 and 2018 (confirmed by laboratory testing). Numbers of cases fell in 2014 and 2015, but rose again in 2016, with 531 measles cases reported - more than five times as many as the total number of cases in 2015. Numbers of cases fell in 2017, but rose again in 2018 (see section 'Key disease facts' above).
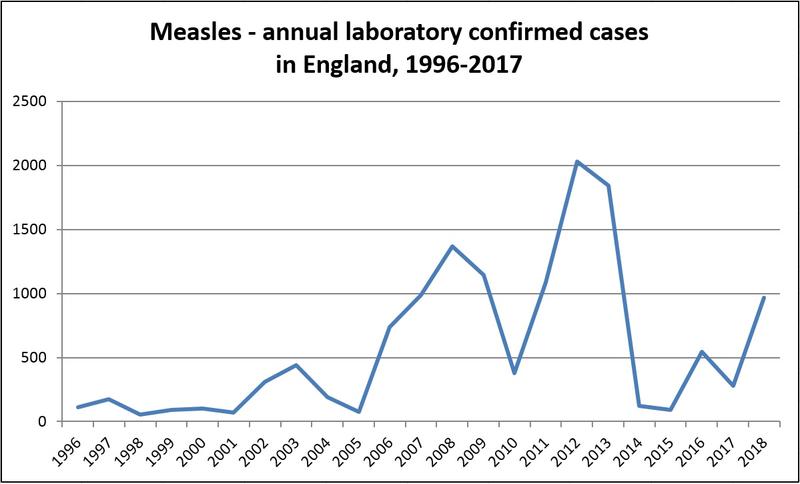
Click here for an accessible text version of this graph Source: UK Health Security Agency and the Health Protection Agency archive |
Vaccines
Page last updated Thursday, June 26, 2025



